
“A mosaic embryo has more than one cell line.” “Think of a mosaic table, they have lots of different rocks or shells,” Flanagan explains. If some (but not all) of the cells they test have different numbers of chromosomes from the magic “normal” number - 46 - the lab report will describe the embryos as mosaic. That’s when your doctor will sample some cells from the TE for testing. Genetic testing of embryos typically occurs during the in vitro fertilization process about five to seven days after an egg is fertilized - when the egg has grown to what’s known as blastocyst stage. The way Jay Flanagan, MD, health expert for the National Society of Genetic Counselors and a clinical associate professor at the University of South Dakota, explains it, embryos are made up of two parts: We’re getting there, and this will all make sense in a moment. Let’s cut through some of the big words that might have been floating around in that doctor’s office, shall we?Ī mosaic embryo is an embryo that has what Emily Jungheim, MD - a reproductive endocrinologist at Northwestern Medicine - calls two more “chromosomally distinct cell lines.” Yes, we know, we said we’d cut out the big words. So, what is a mosaic embryo, and what does this mean for your chances of having a healthy baby? What is a mosaic embryo? But if you just got the news from your fertility clinic that you’ve got a mosaic embryo, you know they’re not talking about aesthetics. Outcome with complementary information from prenatal genetic testing as compared to euploid and non-PGT cohorts.You probably expect the word “mosaic” to show up when you’re searching Pinterest for a new art project to brighten your bedroom walls…not so much when you’re sitting down with your fertility specialist to talk about your embryos. This is the first multi-center prospective study reporting a full MET pregnancy Longitudinal investigation on one MET pregnancy evidenced the aneuploidy depletion hypothesis. All 37 MET live births were confirmed viable, among which 8 completed prenatal genetic testing with normal results. 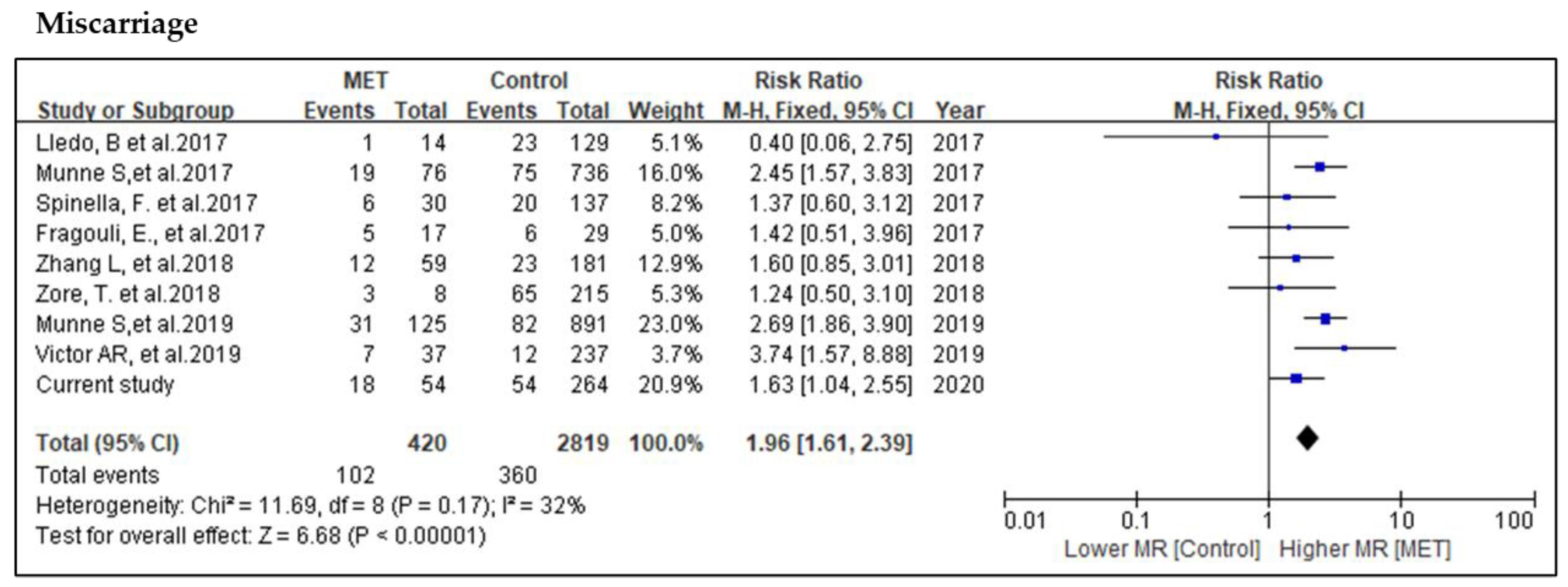
Our meta-analysis concluded that METs gave rise to pregnancies but were associated with a reduced ongoing/live birth rate and a higher miscarriage rate. Pregnancy losses after METs were different between embryos carrying numerical and segmental chromosomal abnormalities (p = 0.04). Mosaic embryo transfers (METs) resulted in a significantly lower clinical pregnancy rate (40.1% versus 59.0% versus 48.4%), lower ongoing/live birth rate (27.1% versus 47.0% versus 35.1%) and higher miscarriage rate (33.3% versus 20.5% versus 27.4%) than euploid and non-PGT transfers, respectively. 
This is a multi-center prospective cohort study on 137 mosaic, 476 euploid and 835 non-preimplantation genetic testing (non-PGT) embryos from three in vitro fertilization (IVF) providers of three countries in Asia, applying the same preimplantation genetic testing for aneuploidies (PGT-A) reporting criteria. Expanded research is warranted to evaluate its clinical significance. Recent studies provided evidence on the viability of mosaic embryos by reporting pregnancy outcomes. This is the first multi-center prospective study reporting a full MET pregnancy outcome with complementary information from prenatal genetic testing as compared to euploid and non-PGT cohorts.Ĭhromosomal mosaicism is at high occurrence in early developmental-stage embryos, but much lower in those at prenatal stage. Chromosomal mosaicism is at high occurrence in early developmental-stage embryos, but much lower in those at prenatal stage.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
